Advanced Heart Surgery for Children: Early Primary Repair
At Children’s National, we plan treatments with your child’s long-term health in mind. If a newborn needs heart surgery, we intervene early and aggressively to correct defects. This way, the repair or reconstruction grows with your child and he or she benefits from a faster recovery. This approach is called early primary repair.
Many heart programs for children recommend waiting until a newborn is older before performing heart surgery. However, the longer we wait, the more health consequences a child may suffer. We perform surgery on infants so we can give them the best possible start in life:
- More than two-thirds of cardiovascular surgeries we perform are on patients less than 1 year old
- Half of those surgeries are on newborns less than 1 month old
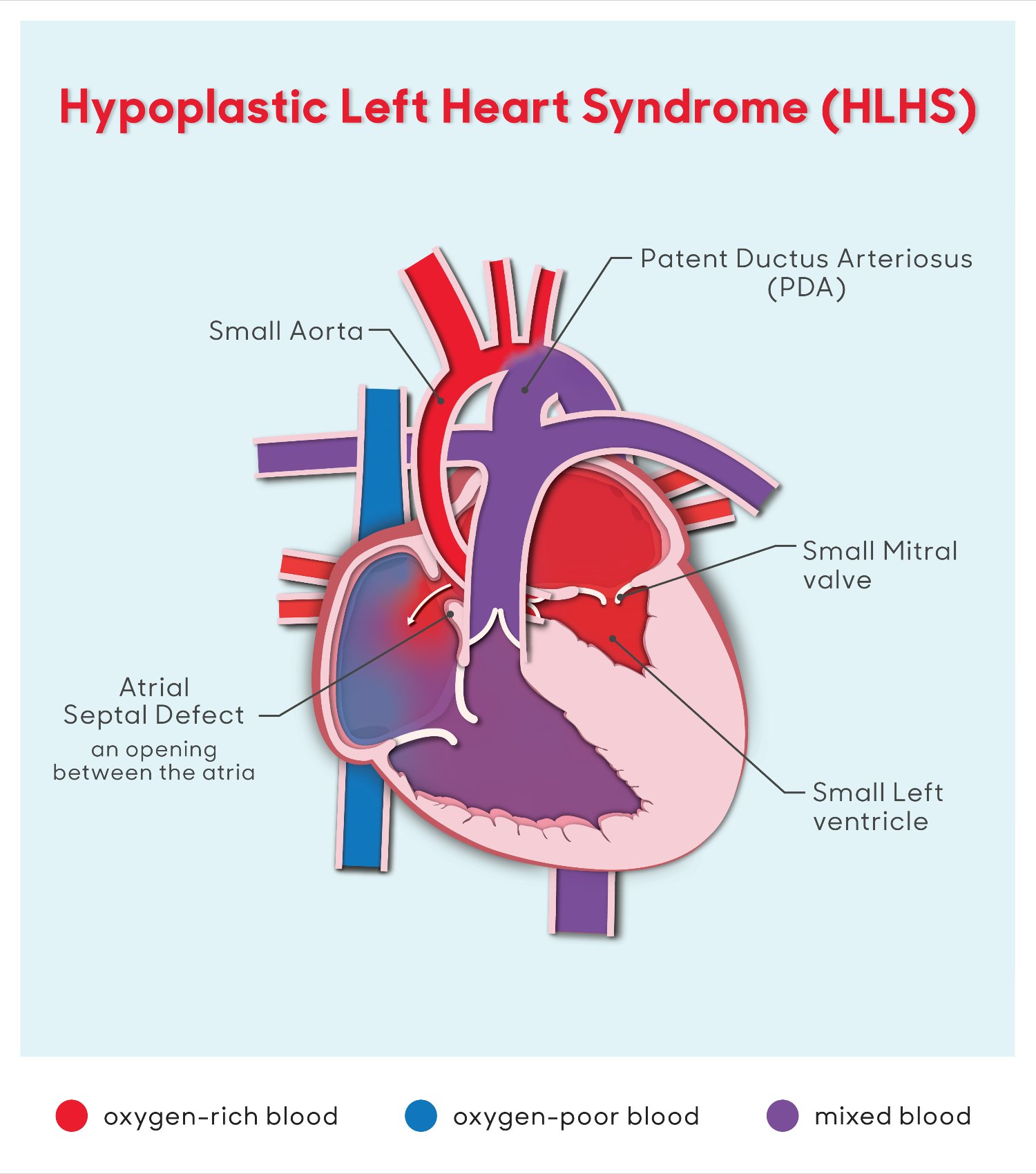
To treat HLHS, multiple surgeries are completed in a staged approach:
Stage 1: The first staged surgery is specific to your child’s anatomy. Your child may undergo a Norwood operation or the HLHS hybrid procedure.
The Norwood procedure is an operation that can either occur within the first few days of birth (this is known as the primary Norwood) or within 3-4 weeks after birth (rapid two stage Norwood). Depending on the type of single ventricle heart defect, different surgical approaches may be used:
- Rapid Two Stage Norwood Procedure:
Children’s National is currently the only hospital in North America performing the rapid two stage Norwood procedure to treat infants with HLHS. In this procedure, infants will undergo rapid bilateral pulmonary artery banding (bPAB) during the first 24 to 48 hours of life. These bands will:
- Help protect your baby’s lungs from getting too much blood flow
- Allow your baby's heart to work more efficiently
- Give surgeons time to plan for the Norwood procedure while your baby grows stronger
While bPAB is performed very quickly after birth, the next stage – known as the Norwood procedure – is typically delayed until 3 to 4 weeks after birth. Traditionally, the Norwood procedure is performed eight (8) days after birth, but there are many advantages to delaying this procedure after bPAB:
- The heart, brain and other major organs have more time to strengthen
- Kidney function improves
- Your baby can begin to breathe and feed on its own
- Allows for more bonding time between the parents and baby
The Norwood procedure is a major open-heart surgery that uses a cardiopulmonary bypass machine (heart-lung machine) to support your baby during the operation.
- HLHS Hybrid Procedure:
The HLHS hybrid procedure is a combination of surgery and cardiac catheterization for babies with HLHS. The goal of the hybrid procedure is to help to delay more complex procedures until your baby grows stronger and healthier.
The hybrid procedure can be performed within the first few days of life. The surgery consists of reducing the blood flow to both lungs using mini-bands around the lung vessels and implanting a special metal stent into the arterial duct to maintain sufficient blood flow to the organs. This approach eliminates the need for the heart-lung machine and a major surgical operation for vulnerable newborns.
Once your child is ready for discharge from the hospital, they will be enrolled in the Single Ventricle Home Monitoring Program. A dedicated nurse practitioner will monitor your child’s progress at home until they receive their Glenn procedure.
Stage 2: Glenn Procedure
The Glenn procedure is an open-heart surgery that typically takes place when your child is between 3 to 6 months of age. The surgeons will connect the superior vena cava, a large vein that carries blue blood from the upper half of the body into the heart, directly to the pulmonary artery. This will enable blue blood from the upper body to flow directly to the lungs, without passing through the heart. If your child had a BTT or Sano shunt, it will be removed since it is no longer needed.
Stage 3: Fontan Procedure
The Fontan procedure can be scheduled any time between 2 and 4 years of age, depending on what your child needs. During this surgery, the inferior vena cava, a large vein that carries blue blood from the lower half of the body into the heart, is attached directly to the pulmonary artery. After the Fontan operation, all of the blue blood will go directly to the lungs without passing through the heart. This takes away a significant amount of work for the single pumping chamber. Given all the advances in surgical care, children born with a single ventricle defect who have completed the Fontan procedure are now living well into adulthood.