Condition
Tetralogy of Fallot (TOF)
What You Need to Know
Tetralogy of Fallot (TOF or "TET") is a condition of several related congenital (present at birth) defects that occur due to abnormal development of the prenatal heart during the first eight weeks of pregnancy.
Key Symptoms
Diagnosis
Treatment
Schedule an Appointment
Our pediatric specialists provide personalized care for your child’s physical, mental and emotional health needs. Meet our providers and schedule an appointment today.
Frequently Asked Questions
Prevention and Risk Assessment
What is tetralogy of Fallot?
What causes tetralogy of Fallot in children?
Why is tetralogy of Fallot in children a concern?
What are the symptoms of tetralogy of Fallot in children?
Diagnosis
How is tetralogy of Fallot in children diagnosed?
Treatment
What is the treatment for tetralogy of Fallot in children?
What postoperative care should I expect for my child's tetralogy of Fallot?
How can I care for my child at home following tetralogy of Fallot repair?
What is the long-term outlook after my child's tetralogy of Fallot surgical repair?
Tetralogy of Fallot Outcomes Data
Explore long-term results for tetralogy of Fallot surgery at Children’s National—from survival to reoperation risk over time.

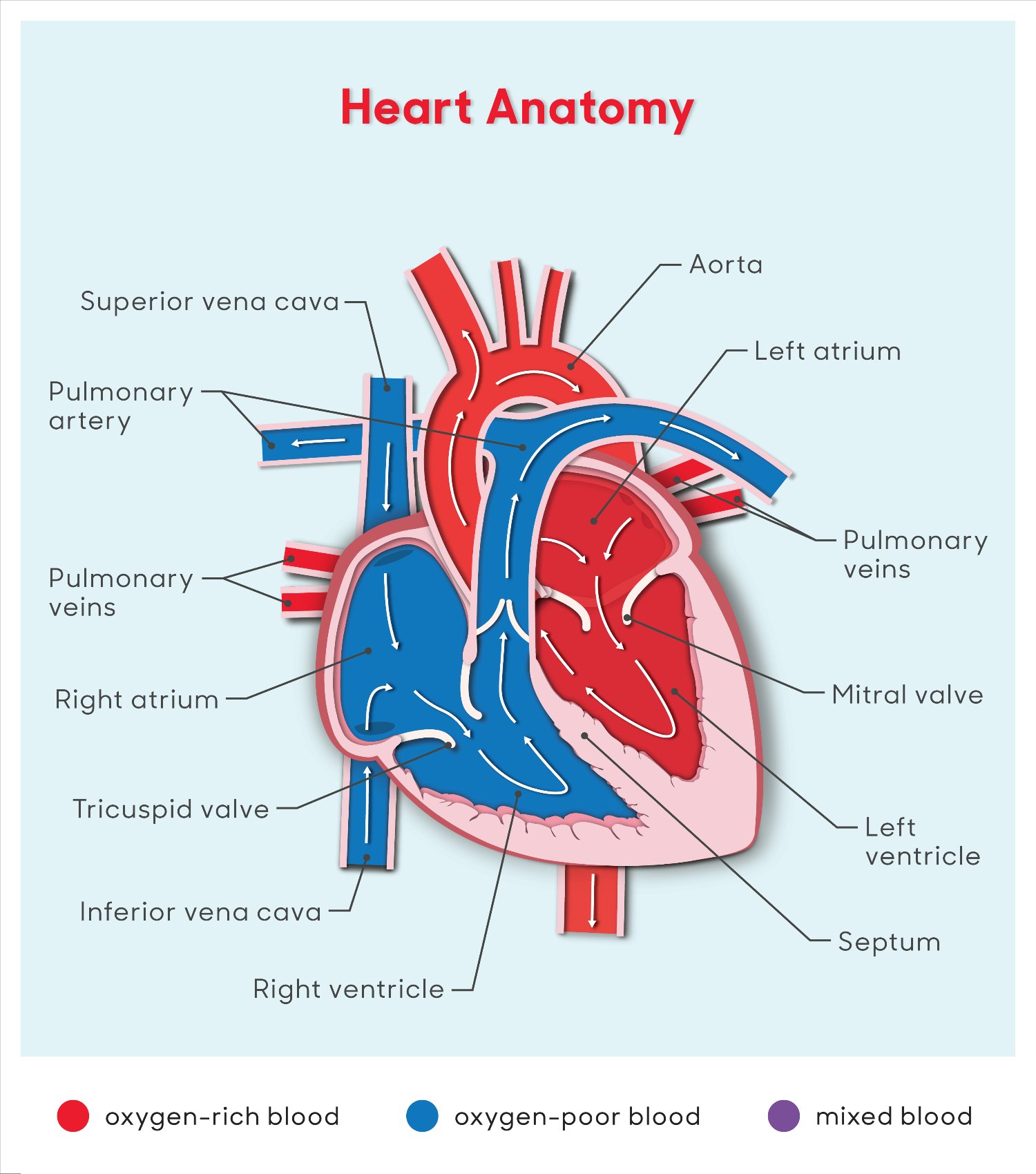
Heart Anatomy Illustration
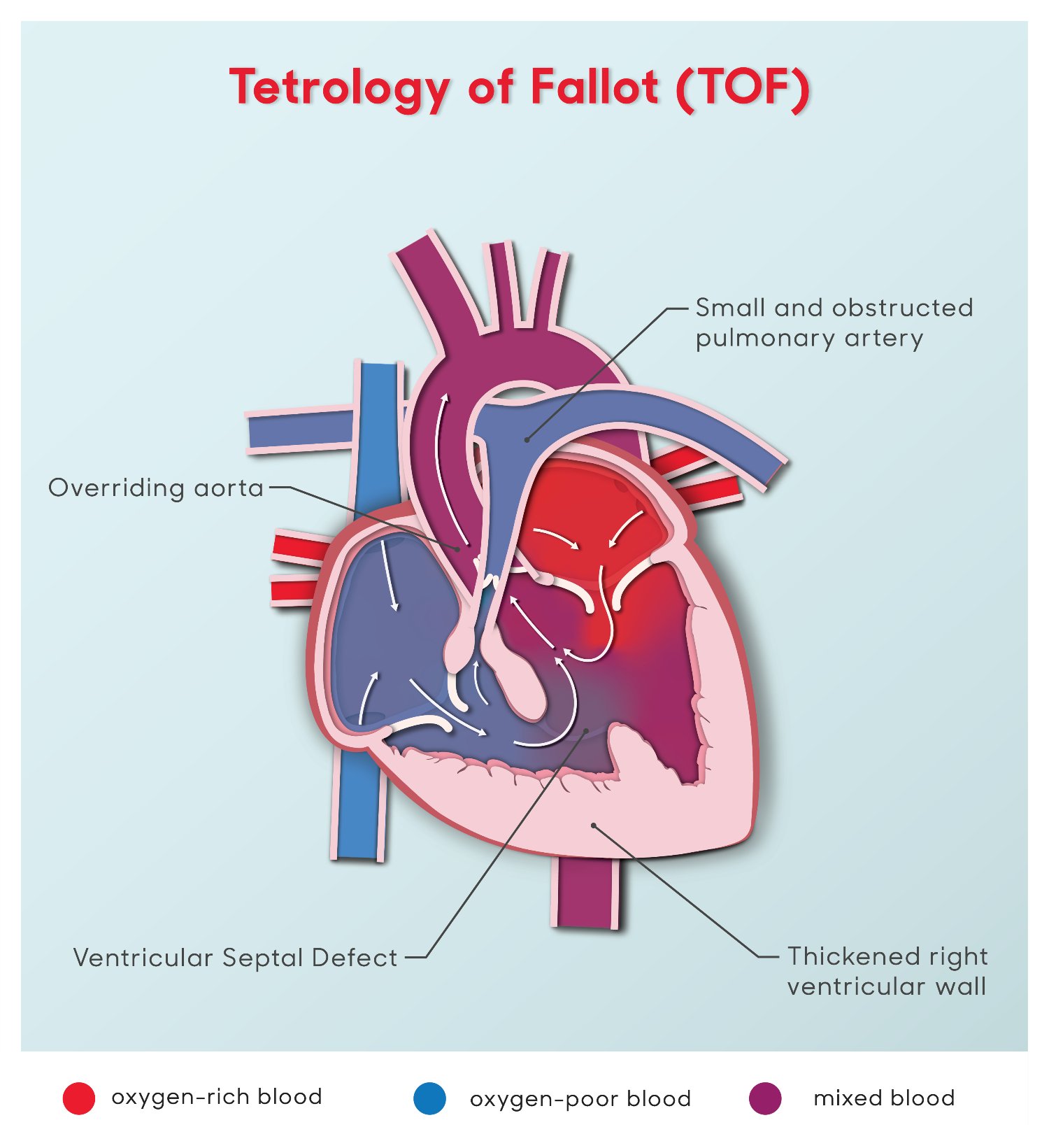
Tetralogy of Fallot Illustration
Meet the Providers Who Treat Tetralogy of Fallot (TOF)
Departments that Treat Tetralogy of Fallot (TOF)

Heart and Lung Center
Our expert pediatric team offers advanced cardiac and pulmonary care, achieving excellent outcomes for thousands of children every year.

Help Kids and Make a Difference
Invest in future cures to help children have brighter futures.