Condition
Newborn Neurologic Disorders
What You Need to Know
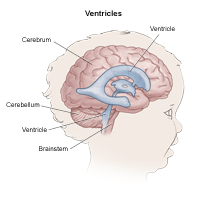
Newborn neurologic disorders are a range of various conditions that affect the brain, spinal cord or nerves. Newborn neurologic disorders usually present at time of birth or develop shortly after. Some forms of newborn neurologic disorders include intraventricular hemorrhage (IVH) and periventricular leukomalacia (PVL).
Key Symptoms
Symptoms for newborn neurologic disorders will vary based on the specific conditions, some known symptoms for IVH are:
- Apnea and bradycardia
- Pale or blue coloring
- Weak suck
- High-pitched cry
- Seizures
- Swelling or bulging of the fontanelles
- Anemia
Diagnosis
In order for doctor's to diagnose newborn neurologic disorders they may perform one or all of the following:
- Complete medical history review
- Physical examination
- Cranial (head) ultrasound
- MRI
Treatment
Treatment for newborn neurologic disorders will vary depending on the specific condition. Most often treatment will include management of problems that could worsen the conditions. Some examples of those treatments are:
- Specialized care
- Physical therapy
- Occupational therapy
- Speech therapy
- Surgery

Schedule an Appointment
Our pediatric specialists provide personalized care for your child’s physical, mental and emotional health needs. Meet the providers who treat newborn neurologic disorder and schedule an appointment today.


Frequently Asked Questions
What is intraventricular hemorrhage (IVH)?
What causes intraventricular hemorrhage?
Why is intraventricular hemorrhage a concern?
What are the different grades of intraventricular hemorrhage?
What are the symptoms of intraventricular hemorrhage?
How is intraventricular hemorrhage diagnosed?
How is intraventricular hemorrhage treated?
What is periventricular leukomalacia (PVL)?
Why is periventricular leukomalacia a concern?
What causes periventricular leukomalacia?
What are the symptoms of periventricular leukomalacia?
How is periventricular leukomalacia diagnosed?
How is periventricular leukomalacia treated?
Departments that Treat Newborn Neurologic Disorders
Neonatology
Whether your infant has arrived prematurely or has a critical illness, the top-ranked neonatology team at Children's National Hospital assists in coordinating every service you and your baby need, including consultations, assessments, emergency treatments and continuing care.

Help Kids and Make a Difference
Invest in future cures to help children have brighter futures.