Colorectal
What You Need to Know About Diagnosing Pediatric Functional Constipation

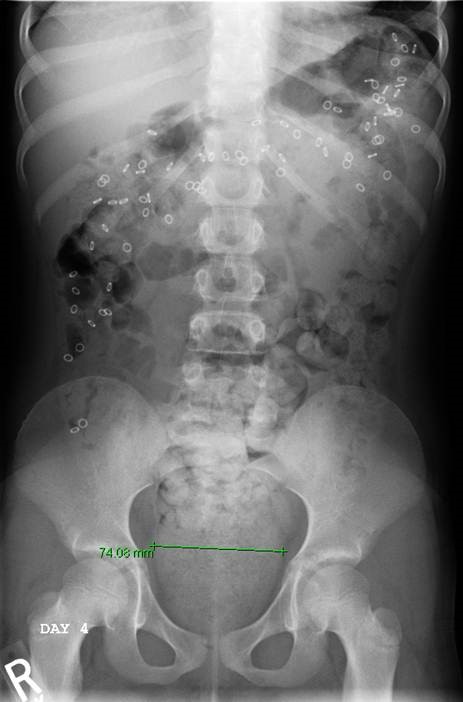
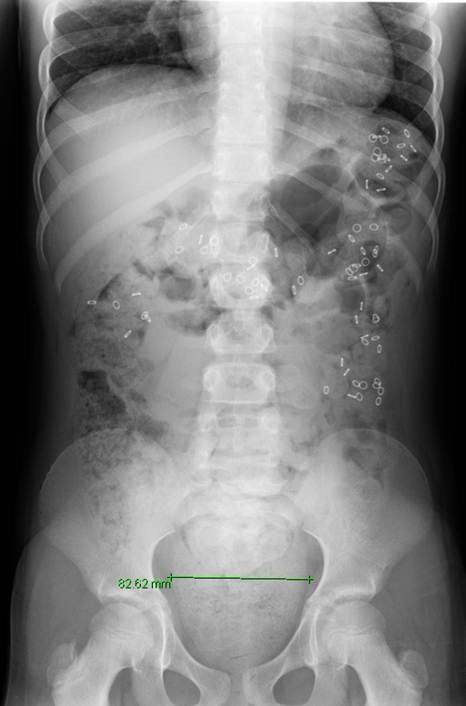
If your child has functional constipation and is not responding well to a bowel management program, pediatric colorectal specialists and gastroenterologists will perform a series of diagnostic tests to determine the underlying cause of the condition.
If your child is a candidate for surgery, the type of surgery your child will need and when to perform it is based on a comprehensive evaluation of the anorectal and colorectal anatomy and physiology.