Mila's Story

The first hour after Mila Vasaio was born was the longest hour of Milena Vasaio’s life.
This second pregnancy had been amazing: Nearly nine months so perfect Milena felt fit enough to run a marathon.
But as soon as Mila was born at 35.5 gestational weeks, it was clear something was terribly wrong. Mila’s breathing didn’t sound right. Milena waited to hear her newborn cry. Her daughter remained eerily silent.
“They were trying to get her going. Nothing was working. They had to rush her to the neonatal intensive care unit (NICU). I don’t know how to explain that feeling. It was such a shock. Luckily, my husband, August, was able to be there. An hour went by. I can’t move. I’m trying to text him. Finally, he texted: ‘She’s OK. They got her breathing.’ Ohmigosh. It really was the longest hour of my life,” Milena says.
After four days in that hospital’s NICU, the staff told the family they had done everything they could. Mila would be flown to Children’s National Hospital, which has a more extensive array of specialists. At Children’s National, Mila underwent examination, diagnostic imaging and genetic testing that revealed a number of health concerns and two diagnoses: Congenital central hypoventilation syndrome (CCHS) and Hirschsprung disease.
CCHS disrupts breathing, making breaths become so shallow that oxygen levels run perilously low and carbon dioxide levels soar too high. The autonomic nervous system is like the body’s own autopilot, ensuring essential tasks like breathing occur automatically so babies, infants and children do not need to remember to breathe in and breathe out. CCHS interferes with those involuntary body processes.
With CCHS, the PHOX2B gene is missing information. This gene provides instructions to proteins that promote nerve cell formation.
In addition, they had been trying to get Mila to progress to a full feeding. She managed to swallow 40 ml, but then she would spit up.
“I remember them looking at X-rays of her upper and lower gastrointestinal tract. One attending doctor, Khodayar Rais-Bahrami, M.D., said ‘Let’s just check her for Hirschsprung disease.’ It doesn’t affect girls as much as boys. Sure enough, my girl. Everything that is rare or uncommon or does not really happen, my child is an example anything is possible─good and bad─because of everything she has gone through,” Milena says.
Mila’s upper gastrointestinal tract looked fine. Timothy Kane, M.D., chief of General and Thoracic Surgery, performed the surgery that checked the length of Mila’s colon, searching for nerve cells known as ganglion cells that help the body transport food through the intestine and relax the colon enough to enable stooling. In most of Mila’s colon, the essential nerve cells were missing.
Mila’s CCHS is so severe that when she sleeps, she stops breathing. A ventilator now does the breathing for her while she dozes. When she’s awake, she breathes in deeply through the tracheostomy and exhales through her nose and mouth. Because her daughter’s lungs are so strong, every so often, Milena can hear Mila’s voice as she cries.
 “We were in tears. She’s not a crybaby,” Milena says. “When I heard her voice for the first time, I wanted to jump out of my skin. It was the best feeling in the world. I don’t ever want to hear my children cry. In this case I was thinking, ‘Please cry.’ I want to hear her voice. It’s rare, but I can hear it. It’s one of the moments I celebrate.”
“We were in tears. She’s not a crybaby,” Milena says. “When I heard her voice for the first time, I wanted to jump out of my skin. It was the best feeling in the world. I don’t ever want to hear my children cry. In this case I was thinking, ‘Please cry.’ I want to hear her voice. It’s rare, but I can hear it. It’s one of the moments I celebrate.”
Mila’s care is managed by the yellow team, and she is seen a consistent team of clinicians and bedside nurses, including Tara Arnold, Erin Clift, Ashley Divelbliss and Fiona Hogan.
“Words could not express our gratitude in how amazing all of the Children’s care teams have been, including doctors, nurses, social workers and respiratory therapists,” Milena says. “They truly, truly love her. That makes a difference when I leave at night and I pick up my son; I feel she is with family. It makes it so much easier to leave her.”
Mila will undergo magnetic resonance imaging to pinpoint what continues to trigger seizures. The family now has learned how to change her trach weekly and her ostomy bag every other day. Mila was prescribed a blood thinner to prevent a recurrence of blood clots; the family now handles those injections. They’re building up confidence with her home ventilator. With a nose filter, a wide-awake Mila can be taken off the ventilator for up to one hour.
She has been hospitalized at Children’s National for nearly 200 days, and on Jan. 12, 2018, Mila turned 6 months old. She’s learning how to hold her head up. Now, Milena is counting the days until her youngest child can go home. “Once she is stable, they’re going to monitor her for a week or two to make sure it’s safe for her to go home,” Milena says.
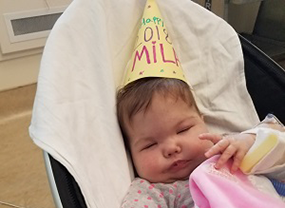
Over New Year’s, they snapped a photo of Mila wearing a festive hat.
“We’re so excited,” Milena says. “We’re starting the New Year off with her in better health with the plan of going home soon. I couldn’t ask for more─beside having her healthy. I feel very blessed to have my daughter getting better and making her way into this crazy world.”
Dr. Chang passed away in June 2022.