Ashley's Story

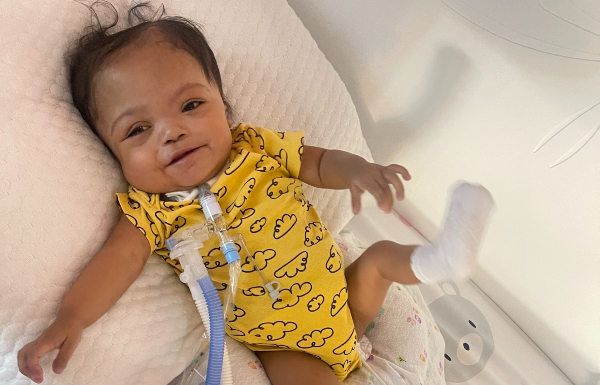
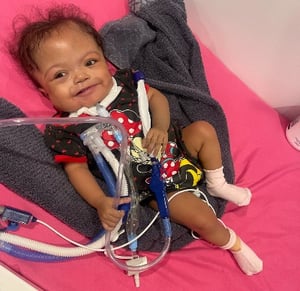 Ashley Vela Mercedes is a happy, smiling 18-month-old. She’s also a true miracle-- the smallest baby in the world with hypoplastic left heart syndrome (HLHS) to survive to this age.
Ashley Vela Mercedes is a happy, smiling 18-month-old. She’s also a true miracle-- the smallest baby in the world with hypoplastic left heart syndrome (HLHS) to survive to this age.
Born when her mom was only 28 weeks pregnant, she was 1.1 kilos/2.4 pounds when she arrived--the size of a beanie baby stuffed animal—and her heart was about the size of a grape.
Between her premature birth and her medical issues including her critical HLHS heart condition, her parents, Ana Mercedes and Axel Vela were told that Ashley was unlikely to survive.
The Velas were frustrated, sad and scared. It started to sound like there wasn’t much hope for their tiny baby. They had always dreamed of having a family of their own. Nothing had prepared them for this.
Hope in The Hybrid Procedure
Their cardiologist wasn’t ready to give up either. She reached out to the team at Children’s National Hospital to see if Ashley might be considered for a new type of surgery—called a “hybrid procedure.” She hoped that this hybrid procedure might stabilize Ashley’s heart until she could grow strong enough for the open-heart surgeries she would need later.
Hybrid heart procedures blend traditional surgery and a minimally invasive interventional, or catheter-based, procedure. A stent is implanted in the newborn’s ductus arteriosus to hold it open and keep the baby’s blood flowing more efficiently. Usually, the ductus serves as a normal fetal blood vessel that increases blood flow to the mother’s placenta while in utero and closes after the baby is born, when it is not needed.
The hybrid procedure to hold open the ductus isn’t a permanent fix—it just buys the baby extra time to grow and develop before open-heart surgery to start rebuilding the heart in a more sustainable way. They are only considered an option for infants at extremely high risk for open-heart surgery. That’s also why very few congenital heart centers in the world offer them.
The hybrid team have worked together on more hybrid procedures for tiny and fragile infants than most other places. They've also worked with the U.S. Food and Drug Administration to safely bring a smaller and more flexible, toothpick-sized stent to the U.S. from Europe that’s made especially for use in the ductus arteriosus of special cases like Ashley.
Record-Setting Smallest Hybrid Surgery
Doctors say that Ashley’s birth weight was too low--she weighed 1.1 kilos or 2.4 pounds--for surgery. Her lungs also were not developed enough. She was so small, she lived in the hospital for several more weeks after birth so she could grow and develop to a size where the hybrid procedure was possible.
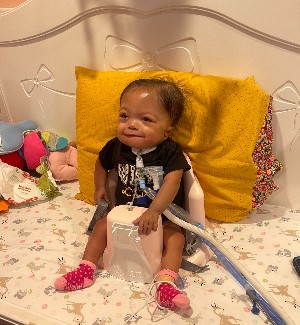
When she reached 1.7 kilos or 3.7 pounds, she was transported to the Cardiac Intensive Care Unit at Children’s National Hospital for her first procedure, the hybrid. At the time, she was officially the smallest baby to have a hybrid procedure at Children’s National. After the surgery, the Children’s National CICU was Ashley’s home for almost her entire first year of life.
“Landing here at Children’s was a blessing because we thought she was going to die. What has happened here is a miracle,” said Ana Mercedes. “I would like to tell [the team] that what they have done with my daughter is incredible, and I will never be able to fully repay them for their efforts.”
Over the next 11 months in the hospital, Ashley had many surgeries and catheterizations, countless other medical procedures and tests, and many, many ups and downs, including some very scary times when she required extracorporeal membrane oxygenation (ECMO) for critical life support.
Celebrating and Thriving at Home
In July 2021, Ashley went home for the first time in her life. She’s monitored jointly by her original cardiologist and the Children’s National single ventricle monitoring program. That program stays in touch with families virtually three times each week. Her care team keeps up with her growth and development through telehealth. Ana Mercedes shares videos and photos of Ashley as part of her routine updates to the clinical team.
She still needs some medical support at home and will likely need additional medical interventions down the road, but for the time being, she is a more independent, happier and thriving little girl.
And she’s a miracle—she is the smallest baby in the world born with HLHS at such a small size and weight to survive to this age.
Ana Mercedes dreams of taking Ashley to the Dominican Republic one day, so they can enjoy the famous beaches and Ashley can be introduced to her heritage since that’s where Ana Mercedes is from.
“We are overall doing well. We have received support from our family and employers,” said Ana Mercedes. “We are extremely grateful to everyone who has given us a hand during this challenging time.”
The last year has been a roller coaster, but Ashley has made incredible progress and exceeded everyone’s expectations. One care provider who knows her noted, “Last year at Christmas time, this little girl was on her fourth catheter procedure and had been in intensive care for her entire life. One year later, she’s at home with her family and celebrating—that’s quite the Christmas miracle.”





