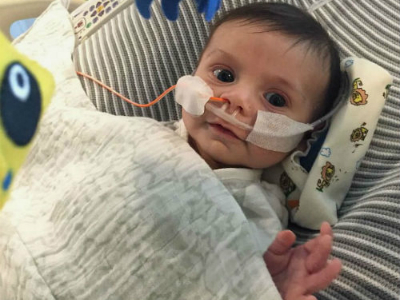
Ryan W.'s Story

In the fall of 2015, Stafford, VA, residents Sarah and Jay gave birth to their first child, a beautiful, healthy baby boy named Ryan.
But when Ryan turned 2 months old, his parents noticed a change in his behavior. Their son – who once loved to eat – suddenly stopped nursing, began sleeping more than usual, gradually became fussy and struggled to breathe when he laid down.
“He just wasn’t himself anymore,” Sarah recalled.
Searching for answers about their son’s condition, Sarah and Jay rushed Ryan to the emergency room at a local hospital where clinicians treated him for dehydration and suggested a follow up appointment with a pediatrician.
With her husband, a pilot in the Marine Corps, away at work, Sarah became increasingly concerned that Ryan’s condition would soon worsen. And when he began gasping for air in his sleep the next day, Sarah called 911 in a panic.
A chest x-ray showed Ryan’s heart was enlarged, and he was transported to the Cardiac Intensive Care Unit (CICU) at Children's National immediately.
“I never in a million years thought that’s why we would be in the emergency room. I thought maybe he had a stomach virus or something else,” Sarah said. “I was pretty much just shocked.”

The next morning, Adam Lowry, M.D., Critical Care Specialist at Children’s National, provided a firm diagnosis: anomalous left coronary artery from the pulmonary artery (ALCAPA), a life-threatening heart defect in which the left coronary artery (which carries blood to the heart) forms abnormally. When the left coronary artery attaches to the pulmonary artery instead of the aorta, the pressure that fills the coronary artery is not adequate – which can cause a baby to have a heart attack.
Two hours after Ryan’s diagnosis, he was scheduled for open heart surgery to correct the defect. The abrupt news brought on a flood of emotions for Ryan’s family.
“I didn’t have any idea the gravity of it,” Sarah said. “It just seemed like my baby who I thought was sick — must’ve been really, really sick because of the way they treated him so quickly. That’s when it sunk in that something big is going on.”
Ryan’s cardiac surgeon and the Cardiac ICU team provided a much-needed sense of relief. They offered regular updates throughout Ryan’s surgery and walked through every detail of his treatment plan.
“We had confidence in the doctors. They communicated with us as much as possible throughout the whole procedure,” Sarah said. “We knew he was in good hands; all we could do was pray and trust everything would be okay.”
Ryan’s surgery was successful, but his medical problems didn’t end there. Now that normal blood flow was established to Ryan’s heart, only time would tell if his damaged heart muscle would recover. Sarah says watching her son spend three weeks in the Cardiac ICU, hooked up to a ventilator and many IVs, was a tremendous challenge. “I wasn’t able to hold him for five days,” she recalled. “That was the hardest part for me. I never left the hospital.”
To get through such a difficult time, Sarah bonded with the clinicians at Children’s National, whom she refers to as “angels.”
“As crazy as it sounds, the ICU for me was a very safe place. I knew Ryan was in very good hands. I really felt like those doctors and nurses saved his life,” she said.
“The nurses always made sure we were a part of the care team when they were making decisions. We felt like they really went out of their way to include us and make sure we understood everything, answering all of our questions.”
With the help of nurses in the Cardiac ICU, Sarah soon experienced the brightest moment of her hospital stay – holding Ryan in her arms again.
“It was a very exciting day,” she said. “I remember sending the picture to family and friends and sharing the news. As a mom, it was something I needed!”
As Ryan gradually got stronger, he spent a week in the Heart and Kidney Unit (HKU) recovering.
After a month-long hospital stay, Ryan returned home where he quickly bounced back to his old self.
“The progress he’s made is just phenomenal,” Sarah said, reflecting on how Ryan – once covered with many tubes – began sleeping and eating regularly. “He’s a very independent guy.”
At 15 months old, Ryan has more than overcome the odds of survival; he’s healthy and thriving.
 Not only is Ryan’s heart function back to normal, he’s hitting his developmental milestones. To celebrate his first birthday, he participated in the Children’s National Race for Every Child 5K and he’s even met former President Obama.
Not only is Ryan’s heart function back to normal, he’s hitting his developmental milestones. To celebrate his first birthday, he participated in the Children’s National Race for Every Child 5K and he’s even met former President Obama.
For Sarah, it’s important that Ryan continue his care at Children’s National with Janet Scheel, M.D., Director of Heart Failure and Cardiac Transplant Program.
“She was with me the day Ryan was diagnosed,” Sarah said, expressing gratitude. “She knows our story and has been on this journey with us.”
Dr. Scheel has a special place in her heart for Ryan, too.
“As a pediatric cardiologist, watching patients like Ryan grow up stronger after a difficult medical journey is one of the greatest gifts of my career. He is an active baby with tons of energy and a bright future, and I couldn’t be more proud,” says Dr. Scheel.


